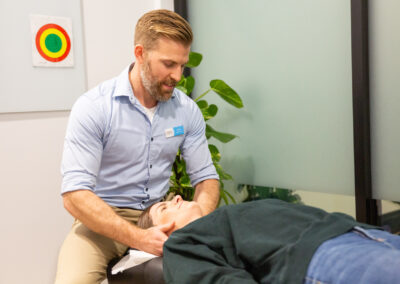
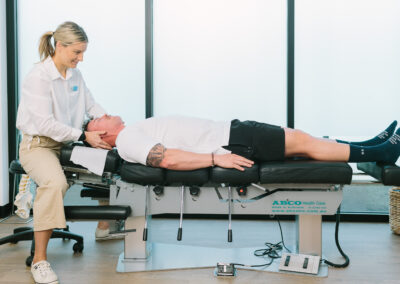
Meet our Chiropractors

Dr. Ryan Bonney
B.Chiro.Sc, M.Chiro, DACNB, DIANM

Dr. Joshua Hallett
B.Chiro.Sc, M.Chiro, DACNB, DIANM

Dr. Jessica O’Keefe
B.Hsc, M.Clin.Chiro

Dr. Daniel Johnstone
M.Clin.Chiro, B.PsySci (Hons), BHSc (Chiro)

Dr. Conor Zyskowski
BHealthSc, BAppSc (Chiro)
Chiropractic
Our chiropractors are dedicated to the diagnosis and treatment of neuromusculoskeletal disorders of the spine.
The human spine is an intricate structure with a degree of complexity that requires expert management.
The Connect Healthcare model has been developed to meet the needs of patients looking for answers to their spine-related conditions ranging from general aches and pains to the more complex of sciatica, balance disorders and headache.
Two of our chiropractors – Josh and Ryan – have completed further specialised training in clinical neurology to become diplomates of the American Chiropractic Neurology Board – a qualification which less than 1% of Australian chiropractors have completed. In 2022, Josh and Ryan became diplomates of the International Academy of Neuromusculoskeletal Medicine (DIANM).
Our approach
If you are looking for answers, our chiropractors are equipped to offer you state of the art treatment directed by the most recent advances in scientific research.
Neuromusculoskeletal diagnosis
Spinal manipulation therapy
Evidence based rehabilitation
Chronic pain management
Soft tissue work
Dry needling
Epley Manoeuvre for positional vertigo (BPPV)
Individualised programs
Competent referral where necessary to the appropriate specialist
Chiropractic FAQs
What will happen on my first visit?
The first consultation will focus on ascertaining a working diagnosis. We will reach this by means of a comprehensive history and a thorough examination.
If we think we can help you, we will let you know immediately, and may often provide some preliminary treatment.
If the complexity of the case requires further testing (X-Rays, MRI, blood tests etc.), we will assist this process.
If your diagnosis requires further management, we will refer you appropriately and liaise with your general practitioner on your behalf.
Please allow 45-60 minutes for this appointment.
What will happen on my second visit?
Once we have garnered the diagnostic information we need, we will discuss with you our treatment approach, your schedule of care, and any treatment modalities we believe will prove useful.
Throughout this process, we strongly encourage questions and concerns you might have. Research shows that the more you understand and actively engage with your treatment program, the better an outcome you can expect.
Please allow 30 minutes for this appointment.
Subsequent consultations
These visits will provide continuing treatment, implementation of corrective exercises,
education on lifestyle modification and behavioural change, and reassessment when
necessary.
Please allow 15-30 minutes for these appointments.
Do I need a referral?
While a number of our patients are referred to us from their general practitioner or a specialist, a referral is not mandatory. However, with Connect Healthcare’s multidisciplinary approach to patient care, practitioners will collaborate with your medical team (where appropriate) to ensure that you receive the best possible health care.
Can I claim on private health insurance or Medicare?
Chiropractic treatments are usually covered by all major private health funds under their ‘extras’ cover. The benefit paid for chiropractic services varies depending on your level of cover and annual limits do apply. For more information, please check with your private health fund.
You may be referred to us by your General Practitioner under the Medicare Chronic Disease Management (CDM) program, previously known as the Enhanced Primary Care (EPC) Program. Under your CDM referral, you will be able to claim a portion of your fees from Medicare, up to a maximum of 5 visits each year.
Our Services
Connect with us
Opening Hours
Mon: 8am - 7pm
Tues: 8:30am - 7pm
Wed: 9am - 7pm
Thurs: 8am - 7pm
Fri: 8:30am - 6pm
Sat: 8am - 12noon
Sun: closed
Schedule a Service or Class
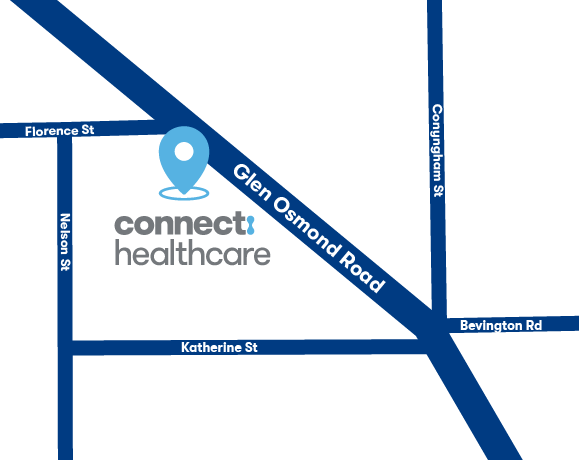
236 Glen Osmond Road, Fullarton, SA, 5063
Parking
Onsite parking is available with lift access to our modern, air-conditioned practice.
Public Transport
We are located 750 metres from the Arkaba Hotel and 150 metres from Bus Stop 6 and 8 on Glen Osmond Road.
Adjacent areas
We provide our allied health services and classes to the Adelaide region, and are conveniently located to the following suburbs - Glen Osmond, Urrbrae, Torrens Park, Unley, Hyde Park, Glenside, Fullarton, Parkside, Burnside, Norwood, St Peters, Payneham, Mitcham, Tusmore, Kensington, Adelaide and Eastwood.
Connect with us
Opening Hours
Mon: 8am - 7pm
Tues: 8am - 7pm
Wed: 9am - 7pm
Thurs: 8am - 7pm
Fri: 8:30am - 6pm
Sat: 8am - 12noon
Sun: closed
Schedule a Service or Class
236 Glen Osmond Road,
Fullarton, SA, 5063
Parking
Onsite parking is available with lift access to our modern, air-conditioned practice.
Public Transport
We are located 750 metres from the Arkaba Hotel and 150 metres from Bus Stop 6 and 8 on Glen Osmond Road.
Adjacent areas
We provide our allied health services and classes to the Adelaide region, and are conveniently located to the following suburbs, Glen Osmond, Urrbrae, Torrens Park, Unley, Hyde Park, Glenside, Fullarton, Parkside, Burnside, Norwood, St Peters, Payneham, Mitcham, Tusmore, Kensington, Adelaide, and Eastwood.
© 2024 Connect Healthcare Group Pty Ltd