Meet our Physiotherapist

Andrew Citti
BPhysio
Andrew Citti is qualified with a Bachelor of Physiotherapy from the University of South Australia, and has experience working in private practice with clients of all ages.
Our approach
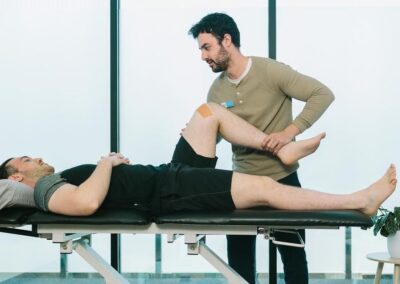
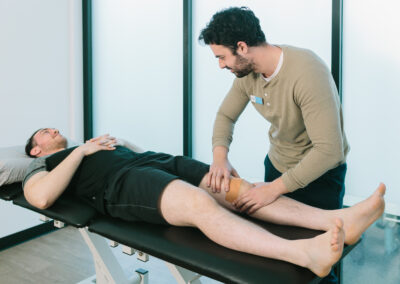
Physiotherapists clinically diagnose and treat individuals in pain or discomfort, but it does not stop there. Here at Connect Healthcare, we utilise hands-on therapy coupled with exercise prescription to not only help reduce pain and discomfort, but to improve overall function and health. Our mission is to empower our clients to be the best version of themselves they can be.
The Connect Healthcare multidisciplinary model has been developed to meet the needs of the client first and foremost, and physiotherapy is a cornerstone to help develop the best level of care guided by the best scientific research. Our treatments and programming are tailored to your needs and goals, in order to support you in taking the next steps to better health.
The benefits
We cater to all individuals no matter how complex or simple the problem, whether you are an elite athlete looking for improvement in performance or taking your first step to better health.
Motion is lotion – let’s get you moving to better health!
Our approach
Some of the treatment methods we utilise include:
Soft tissue therapy
Joint mobilisation techniques
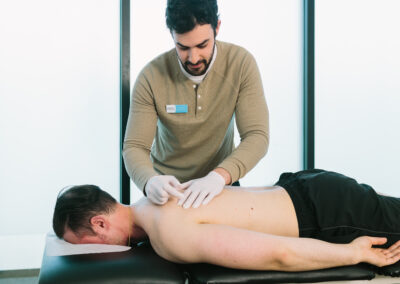
Dry needling
Exercise programming and prescription
Functional movement assessments
Biomechanical assessments (incl. running, golf, gym)
Running assessment
Post-operative orthopaedic care
Physiotherapy FAQs
What will happen on my first visit?
Your first consultulation will focus on ascertaining an accurate diagnosis of your problem. We attain this by discussing the nature of the problem, relevant history and some physical examinations to see where the problem could be stemming from.
It is important to find out what you are looking for and start establishing some goals to help us guide you towards achieving them.
If we believe we can help you, we will tell you and start putting together a plan of how to best manage the problem. If required, we may need to refer for further testing (X-Rays, Ultrasound, MRI for example) or refer you appropriately to other health professionals to help take the best steps for recovery.
Please allow 60 minutes for this appointment.
What will happen on my second and subsequent visits?
Once we establish an accurate diagnosis, we begin implementing a plan to help best resolve the issue. This may change throughout the course of your health journey, but all plans are based upon your goals.
Throughout the journey we will provide hands-on care to help alleviate some of the symptoms you may be experiencing, but research shows that the more you understand and actively engage in your individualised treatment programs, the better outcome you can expect.
We encourage you to ask any questions or concerns you may have along the way.
Please allow 30 minutes for subsequent appointments, but you may be asked to have a longer consultation (45 or 60 minutes) to help best implement your treatment journey.
Do I need a referral?
No. While a number of our patients are referred to us from the general practitioner or specialist it is not mandatory. However, with Connect Healthcare’s multidisciplinary approach to patient care, practitioners will collaborate with your medical team (where appropriate) to ensure that you receive the best possible health care.
Can I claim on private health insurance or Medicare?
Physiotherapy is usually covered by all major private health funds under their ‘extras’ cover. The benefit paid for physiotherapy services varies depending on your level of cover, and annual limits do apply. For more information, please check with your private health fund.
You may be referred to us by your General Practitioner under the Medicare Chronic Disease Management (CDM) Program, previously known as the Enhanced Primary Care (EPC) Program. Under your CDM referral, you will be able to claim a portion of your fees from Medicare, up to a maximum of 5 visits each year.
Do you accept RTWSA, third party insurance (e.g. Motor Vehicle Accident) and DVA referrals?
Yes, we do! If you would like to claim your physiotherapy consultations as part of a RTWSA claim or third party insurance claim, please ensure you bring all relevant documentation (including your claim number, insurance company, and case manager’s name and contact details) to your first appointment.
For DVA clients, please ensure you bring with you a valid referral from your general practitioner for physiotherapy services.
Our Services
Connect with us
Opening Hours
Mon: 8am - 7pm
Tues: 8:30am - 7pm
Wed: 9am - 7pm
Thurs: 8am - 7pm
Fri: 8:30am - 6pm
Sat: 8am - 12noon
Sun: closed
Schedule a Service or Class
236 Glen Osmond Road, Fullarton, SA, 5063
Parking
Onsite parking is available with lift access to our modern, air-conditioned practice.
Public Transport
We are located 750 metres from the Arkaba Hotel and 150 metres from Bus Stop 6 and 8 on Glen Osmond Road.
Adjacent areas
We provide our allied health services and classes to the Adelaide region, and are conveniently located to the following suburbs - Glen Osmond, Urrbrae, Torrens Park, Unley, Hyde Park, Glenside, Fullarton, Parkside, Burnside, Norwood, St Peters, Payneham, Mitcham, Tusmore, Kensington, Adelaide and Eastwood.
Connect with us
Opening Hours
Mon: 8am - 7pm
Tues: 8am - 7pm
Wed: 9am - 7pm
Thurs: 8am - 7pm
Fri: 8:30am - 6pm
Sat: 8am - 12noon
Sun: closed
Schedule a Service or Class
236 Glen Osmond Road,
Fullarton, SA, 5063
Parking
Onsite parking is available with lift access to our modern, air-conditioned practice.
Public Transport
We are located 750 metres from the Arkaba Hotel and 150 metres from Bus Stop 6 and 8 on Glen Osmond Road.
Adjacent areas
We provide our allied health services and classes to the Adelaide region, and are conveniently located to the following suburbs, Glen Osmond, Urrbrae, Torrens Park, Unley, Hyde Park, Glenside, Fullarton, Parkside, Burnside, Norwood, St Peters, Payneham, Mitcham, Tusmore, Kensington, Adelaide, and Eastwood.
© 2024 Connect Healthcare Group Pty Ltd