Meet our Dietitian

Kate Gallasch
APD, ASD, BHlthSc (Hons), BNutDiet
Kate Gallasch is an Accredited Practising Dietitian and Sports Dietitian with 20 years experience.
Eating for better health
Diet can be a way to treat or manage a wide variety of medical conditions, as well as an avenue to improve overall health, wellbeing and lifestyle.
The way we approach nutrition can play a key role in reducing the risk of certain conditions, manage existing conditions, treat symptoms and improve energy, wellbeing and performance in the context of work and concentration, to sports and results driven performance.
Knowing how best to approach nutrition and navigate the vast amount of information that exists in the media and internet can be overwhelming and confusing!
Our dietitian has the expertise and tools to help you find the best approach to reaching your goals whether it be for general health and wellbeing, or for management of specific health conditions. Importantly, our dietitian works with a weight-neutral lens, where focus is placed on engagement in health promoting behaviours, irrespective of body weight, and free from restrictive food rules.
Our approach
In consultations we will discuss the best way to tackle your goals whether that be via dietary counselling, dietary education, eating plans or a combination to best suit your goals and lifestyle.
Please note that meal plans will come at an additional cost.
How we can help
Some examples of what a dietitian may support you in (but not limited to);
General healthy eating advice
Chronic disease management
Sport’s performance – team or individual, recreational or competitive
Mental health nutrition
Gut & digestive health
Women’s health
Vegetarian / vegan diet adequacy
Malnutrition or weight gain
Oncology
Incorporation of the non-diet approach, or a health-focused (not weight-focused) approach
Dietetics FAQs
What is the difference between a dietitian and a nutritionist?
There is often some confusion between the two.
Dietitians are qualified to provide medical nutrition therapy, are skilled in dietary counselling and can provide guidance for the management of medical conditions. Dietitians are trained in evidence-based practice and can help you confidently navigate the nutrition information that bombards us daily in various avenues of media, to choose the best approach for your health. A dietitian, particularly, an Accredited Practising Dietitian (APD) is a registered profession of which indicates over four years of study, professional competency, involves continuing professional development, and is a recognised profession by Medicare, DVA and private health insurers.
Nutritionists may come from a varied background – tertiary qualified nutritionists will study at university for 2-3 years. Qualified nutritionists have expertise to provide nutrition recommendations for general populations and work more so in policy, research, community or organisation-based health. Nutritionists are not qualified to provide information on specific medical conditions.
What will happen on my first visit?
Your first visit will involve obtaining a comprehensive history and understanding of your nutritional concerns/goals to form an assessment. You will be asked to fill out a pre-consult form to best facilitate what we get out of the initial consultation.*
This will lead to a plan being developed, where we can work towards achieving your goals.
If it is identified you may require some further testing such as blood tests, scans or scopes, we will liaise with your other health care providers to facilitate the process, with your consent.
*A link to this form will be provided once you have booked into your initial consultation appointment. You will be asked to complete and return this form at least 24 hours prior to your appointment.
What will happen on my second visit?
In order to get the best out of your diet and dietary goals, it is recommended that there are ongoing reviews of your progress and plan. Nutrition is not one-dimensional and it is beneficial to review and evolve your plan over time to best get results.
In this visit, we can discuss how you may best benefit from reviews, the approach you may like to take, after you have had a chance to process and understand how we may best work together. It’s also a great opportunity to bring along any questions or ideas you may have thought or heard of after the initial consult.
How will it look going forward from here?
Depending on your goal and plan developed, reviews can be 15-45 minutes depending on what we are working to implement and continue with your dietary therapy.
These consults will involve continuing education and support, behavioural and lifestyle modification support, reassessment and management of symptoms reported, motivational interviewing and more.
Do I need a referral?
While a number of our patients are referred to us from their general practitioner or a specialist, a referral is not mandatory. However, with Connect Healthcare’s multidisciplinary approach to patient care, practitioners will collaborate with your medical team (where appropriate) to ensure that you receive the best possible health care.
Can I claim on private health insurance or Medicare?
Dietitian consultations are usually covered by all major private health funds under their ‘extras’ cover. The benefit paid for dietetic services varies depending on your level of cover, and annual limits do apply. For more information, please check with your private health fund.
You may be referred to us by your General Practitioner under the Medicare Chronic Disease Management (CDM) program, previously known as the Enhanced Primary Care (EPC) Program. Under your CDM referral, you will be able to claim a portion of your fees from Medicare, up to a maximum of 5 visits each year.
Our Services
Connect with us
Opening Hours
Mon: 8am - 7pm
Tues: 8:30am - 7pm
Wed: 9am - 7pm
Thurs: 8am - 7pm
Fri: 8:30am - 6pm
Sat: 8am - 12noon
Sun: closed
Schedule a Service or Class
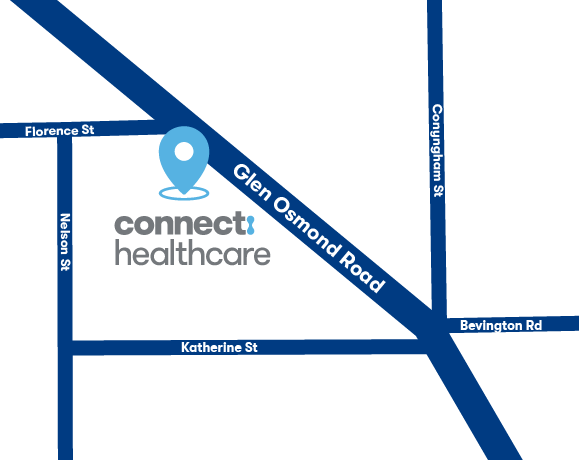
236 Glen Osmond Road, Fullarton, SA, 5063
Parking
Onsite parking is available with lift access to our modern, air-conditioned practice.
Public Transport
We are located 750 metres from the Arkaba Hotel and 150 metres from Bus Stop 6 and 8 on Glen Osmond Road.
Adjacent areas
We provide our allied health services and classes to the Adelaide region, and are conveniently located to the following suburbs - Glen Osmond, Urrbrae, Torrens Park, Unley, Hyde Park, Glenside, Fullarton, Parkside, Burnside, Norwood, St Peters, Payneham, Mitcham, Tusmore, Kensington, Adelaide and Eastwood.
Connect with us
Opening Hours
Mon: 8am - 7pm
Tues: 8am - 7pm
Wed: 9am - 7pm
Thurs: 8am - 7pm
Fri: 8:30am - 6pm
Sat: 8am - 12noon
Sun: closed
Schedule a Service or Class
236 Glen Osmond Road,
Fullarton, SA, 5063
Parking
Onsite parking is available with lift access to our modern, air-conditioned practice.
Public Transport
We are located 750 metres from the Arkaba Hotel and 150 metres from Bus Stop 6 and 8 on Glen Osmond Road.
Adjacent areas
We provide our allied health services and classes to the Adelaide region, and are conveniently located to the following suburbs, Glen Osmond, Urrbrae, Torrens Park, Unley, Hyde Park, Glenside, Fullarton, Parkside, Burnside, Norwood, St Peters, Payneham, Mitcham, Tusmore, Kensington, Adelaide, and Eastwood.
© 2024 Connect Healthcare Group Pty Ltd